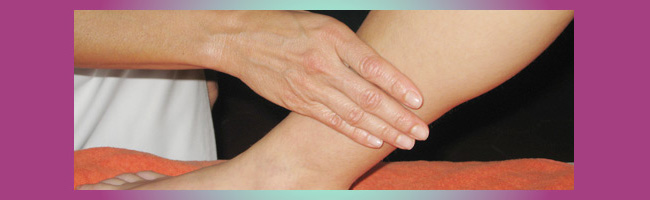
Bendaggio di un linfedema distale (piede e caviglia) in paziente che presenta anche edema cardiaco, utilizzando bende a lunga elasticità.
|
Article 1
From Teachers’ news March 2009 – dr. Vodder School, North America.
* Eric Maus M. D.
From the Department of Internal Medicine, Division of Cardiology University of Texas Health Science Center at Houston and the Hermann Center for Wound Healing and Lymphedema Management, Hermann Hospital, Houston, Texas.
Lymphedema management and Heart Failure
Heart failure could be defined as the inability of the heart to meet the body’s oxygen demand due to decreased contractility of impaired relaxation of the heart walls. When the heart can not efficiently pump, blood can accumulate and lead to congestion within the blood vessels of the lung which can lead to a condition called "pulmonary edema" which is characterized by shortness of breath, cough and chest discomfort among other symptoms. This problem usually worsens when there is an increase in the intravascular volume. Because of this, a history of heart failure has been traditionally considered an absolute contraindication for the performance of complex decongestive therapy in patients with lymphedema. The rational for the contraindication is that mobilizing lymph and compressing the extremities would increase the intravascular volume putting the patient at risk for the development of pulmonary edema. While the contraindication has real pathophysiological basis we consider that some patients with heart failure and lymphedema should be offered complex decongestive therapy under strict medical supervision. On the other side, lymphologists have always advised against the use of diuretics in the management of lymphedema arguing that lymph viscosity can increase with its use and make lymphatic transport more difficult. The purpose of this paper is to discuss the connection between the heart and the lymphatic system in health and disease and to suggest possible alternatives that could be used in the management of patients with these coexistent conditions.
Physiology
The lymph transported by the mayor lymphatic vessels is directed towards the heart via the main thoracic duct ( draining bilateral lower extremities, abdominal and pelvic organs and left upper extremity ) and the lesser thoracic duct that drains the right side of the face, neck and right upper quadrant. These main lymphatic structures drain its content into the left and right subclavian veins respectively and occasionally they can drain also into the internal jugular veins of the respective side. Drainage is facilitated by negative pressure caused by inspiration and by the pumping activity of the lymphatic vessels. The pressure within the above mentioned veins is usually between 0 and 6 mmHg. This is a low pressure system which allows lymph to drain easily from the thoracic ducts into the general circulation. In the presence of heart failure, blood cannot be pumped efficiently out of the heart causing back flow that leads to increased pressure within the venous system. While the thoracic duct can compensate to some extent by increasing the contractile pressure it might not be able to overcome the central venous pressure causing back flow of lymph with progressive development of edema … and in this case, yes, lymphedema. The edema seen in heart failure has not been considered lymphedema but strictly speaking is a very similar phenomenon as what we see with obstructive lymphedema from trauma or surgery where the lymph flow has been interrupted. Here the blockage is functional and not anatomic. In addition to the accumulation of lymph in the tissues, there is water and sodium retention due to hormonal and renal mechanisms that contributes to worsening of the edema. Heart failure can be diagnosed by the physician using physical examination, chest X-Ray, echocardiograms and a blood test called pro – Brain Natriuretic Peptide (pBNP).
Both Problems Coexisting
A good number of patients that present to a lymphedema clinic might have coexisting heart failure. While treatment of heart failure should take precedence, management of lymphedema should not be necessarily withheld. It is well known that untreated lymphedema can lead to various complications ranging from skin ulcers, cellulitis, limb deformity, etc. At the Hermann Center for Lymphedema Management in Huston we have established a protocol to treat patients with compensated heart failure and lymphedema. This has allowed us to provide Complex Decongestive Therapy to several patients that would have been excluded from this treatment somewhere else.
Our Approach
A patient with diagnosis or symptoms suggestive to heart failure is brought to the clinic early in the day. Vital signs are taken and a careful physical examination is performed putting special attention for the presence of abnormal lung and heart sounds and distended neck veins. Weight is recorded and compared to previous weight. Blood is drawn and sent for pro Brain Natriuretic Peptide assessment. This is a marker that is elevated in the presence of heart failure and can help us guide our therapy. A dose of 40 mg intravenous furosemide is administered to reduce the intravascular volume so that the vascular system can accommodate the fluid shift. Patients undergo manual lymph drainage ( MLD ) in the usual fashion and afterwards bandaging of one limb up to the knee is performed. In the presence of bilateral low extremity lymphedema the other limb will be treated once it has been determined the compression is tolerated. The patients are monitored in the clinic for approximately four hours and undergo a repeat pro BNP assay and physical examination prior to discharge if there is significant change in symptoms, pro-BNP level or physical examination the bandages are removed immediately.
Conclusions
Our experience in treating patients with heart failure and lymphedema has been gratifying since the majority of these patients has been able to receive complex decongestive therapy with improvement of their lymphedema. While the approach that we described has not been validated by a randomized double blinded control trial we have seen that the judicious use of compression therapy and manual lymphatic drainage can be used under strict medical supervision in the presence of heart failure. In the presence of lower extremities lymphedema initial bandaging up to the knee will be followed by thigh-high bandaging following day if the patient remained without worsening symptoms. Contralateral leg bandaging can be started in a staged approach as well if needed. We belief that patients with coexisting heart failure and lymphedema deserve the opportunity to be treated. Some patients will not be able to tolerate compression and MLD but we have seen that the majority of patients will adapt to therapy without complications.
|
|
| |
Article 2
CONGRESSO INTERNAZIONALE DI MEDICINA PALLIATIVA
MONTREAL, 27.10.2006
IL LINFODRENAGGIO MANUALE NELLA TERAPIA PALLIATIVA
di Monica Coggiola
Prendersi cura di un paziente oncologico, in particolar modo quando si è consapevoli che si tratti di una terapia palliativa, significa accompagnare un Essere Umano durante una fase molto delicata e difficile della propria vita.
Il trattamento, effettuato su specifica prescrizione medica, dovrà essere
particolarmente adattato allla situazione, sia per ciò che riguarda l’ambiente nel quale si svolgeranno le sedute, sia per l’estrema delicatezza che dovrà caratterizzare la nostra manualità.
In questi casi, è indispensabile avere a disposizione una camera tranquilla ed appartata, per garantire la giusta privacy, l’assenza di altri pazienti trattati in concomitanza e comunque un fastidioso via vai di persone, seppure
operatori sanitari.
Si avrà cura di posizionare il paziente nel modo più confortevole possibile,
avvalendosi delll’utilizzo di cuscini e di teli e coperte per coprire le zone del corpo sulle quali non si sta operando.
Il LDM secondo Vodder non deve mai provocare arrossamento e, meno che mai, dolore.
E’ interessante notare che questa tecnica risulta efficace anche nella situazione in cui non sia possibile toccare direttamente la zona edematosa, a causa della presenza di problematiche locali come piaghe, metastasi, cute danneggiata da radioterapia recente, ecc…
Il LDM è un massaggio riflesso, che ci permette, infatti, di effettuare un trattamento efficace pur lavorando a distanza, attivando dapprima le stazioni terminali del sistema Vascolare Linfatico (il cosiddetto "Terminus", posto alla base del collo, bilateralmente, alla confluenza tra vena giugulare e succlavia) e, successivamente, le zone limitrofe, seguendo la direzione delle vie fisiologiche di deflusso linfatico della pelle e, nelle situazioni nelle quali questo non sia possibile, attraversandole.
Con questa tecnica, suscitiamo un’onda peristaltica a livello dei vasi linfatici, otteniamo inoltre un effetto detto "simpaticolitico" che induce nel paziente un estremo rilassamento, al punto che molte persone scivolano dolcemente nel sonno.
Un altro effetto del LDM è di sedazione del dolore, tale effetto è basato sul fatto che, con le nostre manualità, stimoliamo i recettori del contatto (meccanorecettori) della cute, che sono antagonisti dei recettori del dolore (nocicettori ), secondo la Teoria del Cancello (Gate Control. Melzach & Wall, 1966).
Gli effetti del LDM sono stati dimostrati scientificamente, e, anche in caso di terapia palliativa, siamo in grado di offrire il nostro contributo ai fini del miglioramento della qualità di vita del paziente, anche se non si possono paragonare i risultati ottenibili in queste situazioni con quelli che si possono invece riscontrare in caso di linfedemi benigni.
Al LDM farà seguito il bendaggio dell’arto edematoso.
In terapia palliativa, la pressione effettuata dal bendaggio dovrà essere ridotta rispetto a quella utilizzata nel bendaggio di un linfedema benigno, per non provocare alcun disagio.
Si tratta di una terapia palliativa nel vero senso della frase… "Mettere un mantello sul problema" (dal latino pallium = mantello).
Segue la spiegazione con dimostrazione pratica del trattamento con Linfodrenaggio Manuale secondo Vodder e bendaggio elastocompressivo (eseguito con bende a corta elasticità ed imbottitura) dell’arto superiore di una paziente affetta da infedema secondario post - mastectomia.
Nei trattamenti palliativi i nostri movimenti ed i bendaggi saranno "adattati" con cura, per ciò che riguarda la pressione effettuata, alla sensibilità ed alla tolleranza del paziente.
Il trattamento di un paziente nella fase finale della vita richiede sicuramente, da parte del terapista, doti di fine sensibilità. Infatti, l’operatore dovrà trovare il giusto equilibrio tra compassione e distacco, e mostrare un corretto atteggiamento di calorosa simpatia.
|
|
|


|

Article 3
BRITISH LIMPHOLOGY SOCIETY BLS NEWS AND VIEWS EAST MIDLANDS EDITION September / October 2009 Issue 74.
By Silvia Giolo, Specialist Physiotherapist in Lymphoedema, St George’s Healthcare NHS Trust, London
The treatment of Lymphoedema Filariasis
In March this year, I took the opportunity to spend two weeks at the Institute of Applied Dermatology (IAD), in Kasaragod (Kerala, India). The Institute, directed by Dr Narahari, treats one of the most disabling and disfiguring condition of the world: Lymphoedema Filariasis (LF).
IAD uses an integrated approach in the treatment of Lymphoedema Filariasis, which comprises of allopathy, ayurveda, yoga, homeopathy and physiotherapy. This has allowed creation of a patient centred, self-care, home-based and therefore low cost treatment. Unfortunately, Lymphoedema Filariasis mostly affects the poorest populations in the poorest regions, thus even a low cost treatment is unaffordable for most patients.
My role was not to teach lymphoedema management, but to collaborate with the team, observe their treatment and learn from each other. The intention was to show the techniques used in the western countries and learn the ones used in Kerala; to collaborate with the team to implement treatment plans and identify possible solutions to overcome common difficulties.
At present, IAD has 8 beds for in-patients in a ward of a local hospital. However, the plan is to open their own hospital in order to be able to meet the increasing request for help. Patients are admitted for 7-21 days, and then continue the treatment at home, being followed up after one, 3 and 6 months.
The treatment starts with the education of patient and relatives on the cornerstones of lymphoedema management. Each patient receives at least one to two hours counselling on admission, discharge and follow up.
Skin care combines elements of biomedicine (antiseptic soaps and antifungal creams) and elements of the ayurvedic tradition (Phanta soaks). Then the patient performs Pre-Treatment Yoga, (without bandages on), followed by modified Ayurvedic massage (Unmardhana – dry massage, Udhvarthana – oil massage) and, in selected cases, Swedana (steaming process with selected ayurvedic oils). The choice of the Ayurvedic drug is made on the basis of the local clinical manifestations (Vikruthi of the patient). Subsequently, the patient receives Compression Bandaging and performs Post-Treatment Yoga (with bandages).
Finally, patients are requested to follow a strict vegetarian diet and specific food restrictions.
After the first few days, a patient’s relative is taught how to apply the bandages and perform the massages. He will then treat the patient on a daily basis, together with the therapist, in order to learn the technique and continue at home. This empowers the patient and not only enhances self management but also hugely reduces treatment costs. The sense of family is very strong in India, and relatives live in the hospital with the patients and are actively involved in their care.
During my stay, I spent most of the day working with the team, learning their techniques, exchanging ideas and expertise. We had several “brainstorming” meetings, coordinated by Dr Narahari, to discuss the rationale behind different techniques of lymphoedema management in Europe and compare them with the integrated treatment of IAD.
Interestingly, Yoga may substitute our concept of Manual Lymph Drainage in terms of opening the proximal lymphatic pathways, and stressing on deep breathing to enhance lymph flow. Moreover, our manual techniques for Lymph Drainage are replaced by “modified ayurvedic massage”: deep and firm massage from the ayurvedic tradition, modified in order to follow the lymph pathways (Ayurvedic massage for limbs is normally carried out following a proximal to distal sequence, whereas in LF it is distal to proximal) and performed using medicated or non medicated oils according to the Vikruthi of the patient. Yoga also incorporates great part of classic Physiotherapy exercises. However, a Physiotherapist has recently joined the team, thus we took the opportunity to review and implement assessment and exercise protocols for lower and upper limb oedema.
I was mostly impressed by the way IAD has managed to create a really patient centred approach, identifying what the local resources are, but also considering the social and cultural background of patients and carers. IAD team is exceptionally open to learn any treatment that could improve their protocol.
It was very interesting trialling MLD on some selected patients, mainly those with root limb and genital oedema, and the team showed great interest in learning the technique and trialling it, including instructing selected patients on Simple Lymphatic Drainage. In particular, this was taken on board as a good tool for arm lymphoedema, as IAD experience mostly comes from the lower legs, thus secondary lymphoedema caused by cancer treatment creates more difficulties.
This open view is crucial for improving quality of care: with lymphoedema still being an open field for research, countries certainly have a lot to learn one from each other.
The real challenge, though, was to adapt treatment suggestions to what was available and achievable locally (Potassium permanganate
soaks in the UK may be as cheaper as Phanta soaks in Kerala; however, we may not be able to afford Phanta soaks, and vice versa!)
Ideal treatment is useless if economical, cultural and physical resources are not available. As an example, using padding to improve the limb’s shape is common practice in Europe, but the oil of the ayurveda damages the foam very easily, and the hot weather provokes sweating and skin reactions. Material needs to be strong enough to be sterilised and re-used several times, and bandages need to last as long as possible. Furthermore, short stretch bandages are not available or are very low in quality, thus IAD mainly uses long stretch bandages or short stretch donated by western companies, when possible. Moreover, as garments are not available, patients need to continue using bandages lifelong.
Unfortunately, bandages and products from the biomedicine remain the main expenses faced by the patient. If we think that one bandage may be as expensive as one month salary, we easily understand
the economical burden that LF has on patients who usually come from the poorest areas, who cannot work because of their condition and can hardly walk due to the extent of their swelling. These patients are in real need of treatment, thus the necessity of finding a home-based, self-care treatment, and to reduce its costs to a minimum.
I must admit, I was really amazed by the results obtained, not only in two – three weeks of intensive treatment but also in the long term management and in the volume reduction maintained at follow ups.
In the last few days of my stay, I released an interview for the regional TV channel, Kasaragod Vision, as well as for a regional newspaper. In both occasions, the aim was to explain the cornerstones of lymphoedema management, the treatment for Lymphoedema Filariasis in India, the differences and analogies with the management in the western countries, etc.
The goal was not only to raise awareness in LF, but also to demonstrate to professionals and governmental bodies that the treatment carried out at IAD is as valuable as the one provided in developed countries.
Moreover, I was asked to run a teaching session on the management of lymphoedema to a hundred student nurses, as part of their CPD programme.
Finally, I took the opportunity to teach the use of arterial Doppler, generously donated by Huntleigh Healthcare. Although Doppler assessment is obviously not achievable on LF patients, IAD also treats those with leg ulcers and arterial disease, thus they welcomed the opportunity to learn and use this new skill.
Words are too little to describe this fulfilling experience; I really felt part of the team, in only two weeks I felt as if I had a family there: colleagues, friends and patients, without mentioning the family who was expecting me at home every night. Brijesh and his parents warmly welcomed me from the first day of my arrival, and made me feel at home straight away. On Sundays, I was also shown the amazing province of Kerala, with its numerous temples, extraordinary art and culture.
I would like to thank Dr Narahari, Dr Bose, Vivek and all the team, for the creating such a professionally challenging and in the meantime human and friendly environment.
Finally, I would like to thank BSN Medical, Haddenham Healthcare and Activa Healthcare for the support provided and the material given. Once again, the gratitude in the eyes of the patients is hardly communicable in words.
For further details on the Institute of Applied Dermatology visit www.indindermatology.org or contact Silvia via e-mail at silvia.giolo@stgeorges.nhs.uk

|